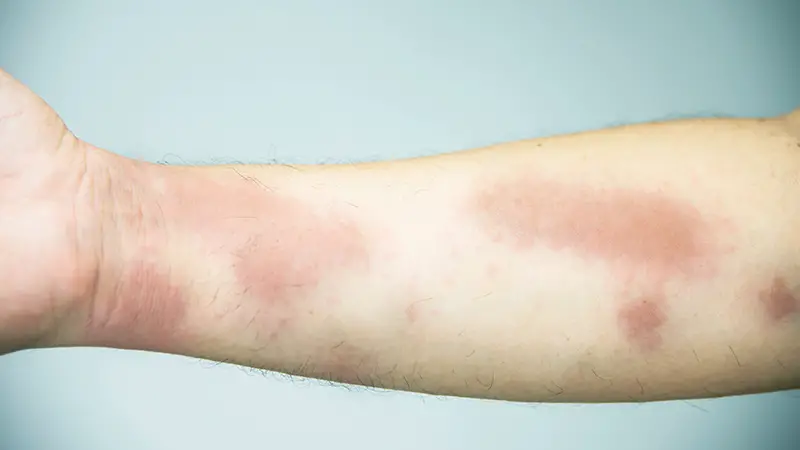
Diabetes is a complex and prevalent metabolic disorder that affects millions of individuals worldwide.
Beyond its more widely recognized complications, such as high blood sugar levels and cardiovascular issues, diabetes can also influence various aspects of daily life, including how the body responds to injuries.
A puzzling phenomenon for many diabetic individuals is the increased tendency to bruise easily. While bruises are common for everyone, diabetics often find that they occur more readily and with distinct characteristics.
This phenomenon sparks curiosity about why diabetics bruise easily and what factors contribute to this vulnerability.
In this exploration, we delve into why do diabetics bruise easily what makes individuals with diabetes more prone to bruising, and provide insights into how to address and manage this unique challenge.
Why Do Diabetics Bruise Easily?
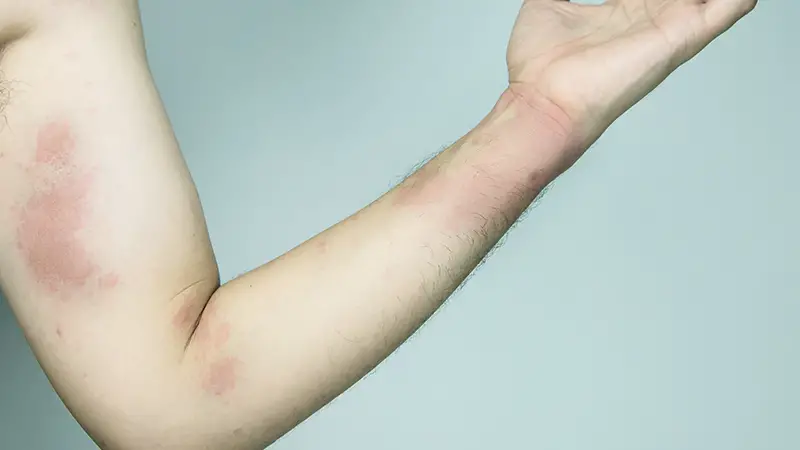
Diabetics often experience a higher propensity to bruise easily due to various factors related to their condition.
Here are the reasons why this happens:
Impaired Blood Vessel Function
Diabetes can damage blood vessels and impair their ability to constrict and expand properly. This vascular dysfunction reduces the body’s ability to respond to injuries, making blood vessels more fragile and susceptible to rupture, leading to easier bruising.
Blood Clotting Abnormalities
Diabetes can disrupt the balance between the blood’s ability to clot and prevent excessive bleeding. This imbalance may result in a tendency to form smaller clots, contributing to easier bruising when minor injuries occur.
Skin Changes
Diabetes can lead to skin changes such as thinning, drying, and reduced elasticity. Weakened skin is more susceptible to injury, and even minor trauma that might not cause bruising in others can result in bruises for diabetics.
Microangiopathy
Diabetics can develop a condition called microangiopathy, characterized by damage to small blood vessels throughout the body. This can result in the fragility of the capillaries, making them more prone to leakage and bruising.
Reduced Platelet Function
Platelets play a crucial role in blood clotting. Diabetes can affect platelet function, making the clotting process less efficient, which can lead to increased bruising even from minor incidents.
Medications
Some medications used to manage diabetes, like aspirin or anticoagulants, can further increase the risk of easy bruising. These drugs may interfere with blood clotting mechanisms.
Poorly Controlled Blood Sugar
Fluctuations in blood sugar levels, especially frequent episodes of high blood sugar (hyperglycemia), can weaken blood vessels and reduce the body’s ability to heal minor injuries. Poorly controlled diabetes exacerbates the risk of bruising.
Managing diabetes effectively through lifestyle changes, proper medication, and regular monitoring can help mitigate these risks and reduce the likelihood of experiencing frequent and severe bruising.
It’s important for diabetics to consult with healthcare providers for personalized advice on managing their condition and associated symptoms like easy bruising.
What Does A Diabetic Bruise Look Like?
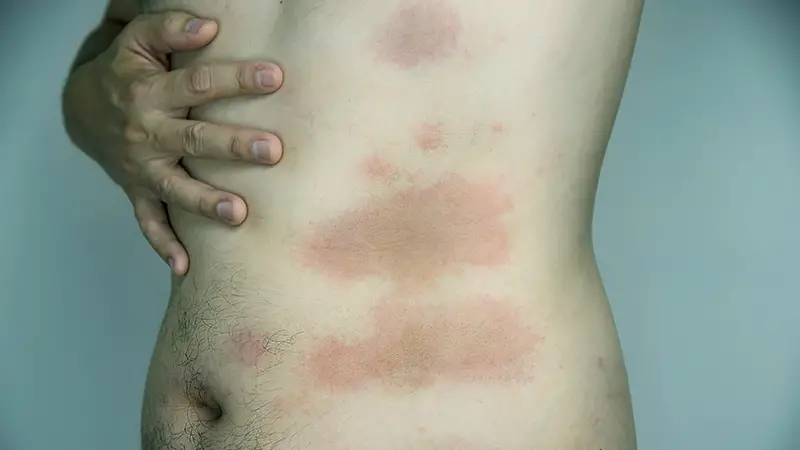
Bruising in individuals with diabetes can vary in appearance, just like in people without diabetes. However, due to certain factors related to the condition, diabetic bruises may exhibit distinct characteristics.
Here are the types of bruises and their descriptions:
Purple or Blue Bruises
The most common type of diabetic bruise resembles the typical purple or blue discoloration observed in non-diabetic individuals. These bruises result from ruptured blood vessels under the skin, causing the pooling of blood, leading to these classic hues.
Large, Spreading Bruises
Diabetic bruises can often appear larger and spread out more than expected. This occurs because damaged blood vessels may take longer to heal, allowing the bruise to expand in size over time.
Delayed Onset Bruises
Some diabetics may notice bruises appearing with a delay after the initial injury, even if the injury seemed minor. This delayed onset is due to compromised blood vessel function, which can affect the body’s ability to respond promptly to trauma.
Yellow or Greenish Bruises
As bruises heal, they can transition from purple or blue to yellow or greenish colors. Diabetic bruises may take longer to reach this healing stage, contributing to their distinctive appearance.
Painful Bruises
Diabetic bruises can sometimes be more painful than bruises in non-diabetic individuals. This heightened sensitivity may be related to nerve damage (neuropathy) often associated with diabetes.
Harder, Lumpy Bruises
Diabetic bruises may feel harder and more lumpy to the touch due to changes in the composition of the surrounding tissue, which may affect the way the bruise forms and heals.
Frequent Recurrence
Diabetic individuals might experience recurrent or frequent bruising, even from minor bumps or pressure. This is attributed to the combination of blood vessel fragility and delayed healing.
It’s important to note that while these characteristics can be more common in diabetics, not all individuals with diabetes will exhibit these traits in their bruises.
If you have concerns about bruising or notice any unusual changes, it’s advisable to consult a healthcare provider to rule out underlying issues and receive appropriate guidance on diabetes management.
How To Treat Diabetic Bruises?

Treating diabetic bruises involves a combination of strategies to promote healing and prevent further injury or complications.
Here are some treatment approaches for diabetic bruises:
RICE Method
The RICE method, which stands for Rest, Ice, Compression, and Elevation, can be effective for managing diabetic bruises.
Rest the affected area to prevent additional injury, apply ice to reduce swelling and pain, use compression with an elastic bandage to minimize blood pooling, and elevate the bruised area above heart level to aid in drainage and reduce swelling.
Topical Ointments
Over-the-counter topical ointments containing ingredients like arnica or vitamin K may help reduce bruising and promote healing. Apply these ointments as directed on the package to the affected area.
Avoid Aggravating Factors
Prevent further injury or damage to the bruised area by avoiding activities that could lead to additional trauma.
Be cautious with tight clothing, and ensure that shoes or footwear are comfortable to minimize pressure on the feet and lower extremities, which are common sites for diabetic bruises.
Hydration and Nutrition
Staying well-hydrated and consuming a balanced diet rich in nutrients like vitamin C, which is important for collagen production, can aid in the body’s natural healing process. Adequate hydration is essential for maintaining skin health.
Monitor Blood Sugar Levels
Managing blood sugar levels is crucial for reducing the risk of diabetic complications, including poor wound healing. Keep blood sugar within target ranges through diet, medication, and regular monitoring to support overall healing.
Wound Care
If the bruised area becomes an open wound or ulcer, proper wound care is essential. Keep the wound clean, apply antiseptic as directed, and cover it with sterile dressings.
Consult a healthcare provider for guidance on advanced wound care if necessary.
Medical Evaluation
If you notice frequent, severe, or unusual bruising that doesn’t seem related to injuries, it’s important to consult a healthcare provider. It could be a sign of underlying issues like blood clotting disorders or compromised vascular health.
Your healthcare provider can perform tests and offer guidance on managing these concerns.
While these treatment strategies can help manage diabetic bruises, it’s essential to remember that prevention is often the best approach.
Managing diabetes effectively, maintaining a healthy lifestyle, and taking precautions to avoid injury can significantly reduce the occurrence of bruises and support overall well-being.
What Are Some Diabetes And Other Skin Problems?
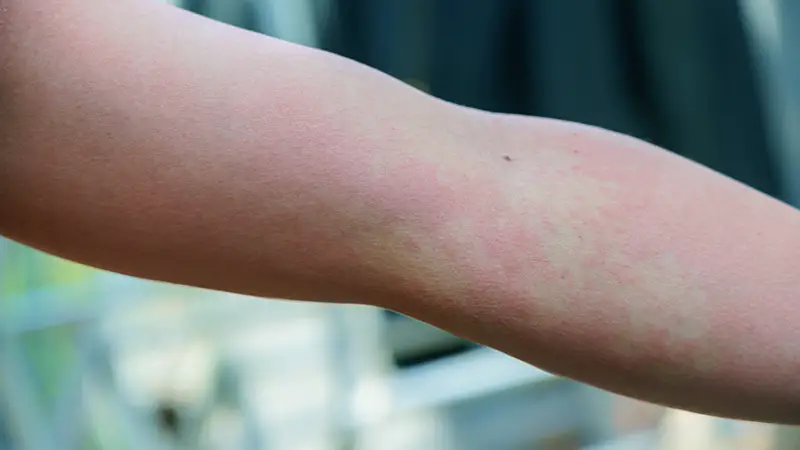
Diabetes can affect various organ systems in the body, including the skin. Here are some common skin problems associated with diabetes:
Diabetic Dermopathy
Diabetic dermopathy is a common skin condition characterized by light brown or reddish, round or oval patches on the skin. These patches are typically scaly and do not itch or hurt.
They often appear on the shins and are thought to result from changes in small blood vessels due to diabetes.
Acanthosis Nigricans
Acanthosis nigricans presents as dark, thickened, and velvety patches of skin, typically in body folds, such as the neck, armpits, and groin. It is associated with insulin resistance and can be a sign of prediabetes or Type 2 diabetes.
Skin Infections
People with diabetes are more susceptible to skin infections, including bacterial, fungal, and yeast infections. These infections can occur in various areas of the body and may require topical or oral treatments.
Diabetic Blisters (Bullosis Diabeticorum)
Diabetic blisters are rare, fluid-filled blisters that can appear on the backs of fingers, hands, toes, feet, and occasionally, the legs or forearms. They are painless and typically heal on their own without treatment.
Xerosis (Dry Skin)
Diabetes can lead to dry skin, which may cause itching, cracking, and even skin sores. Proper hydration, moisturizing, and avoiding harsh soaps can help manage dry skin associated with diabetes.
Necrobiosis Lipoidica Diabeticorum
Necrobiosis lipoidica diabeticorum is a rare skin condition characterized by yellowish, waxy patches on the skin, often on the shins. These patches can become ulcerated and may require medical attention.
Digital Sclerosis
Digital sclerosis is a condition in which the skin on the fingers and toes becomes thick and waxy. It can make finger movement difficult and may be associated with poorly controlled diabetes.
It’s important for individuals with diabetes to monitor their skin carefully, maintain good blood sugar control, and seek prompt medical attention if they notice any unusual skin changes or problems.
Effective diabetes management and a healthy skincare routine can help reduce the risk and severity of these skin issues.
FAQs
Why do diabetics bruise more easily than others?
Diabetics may bruise more easily due to multiple factors. Diabetes can lead to impaired blood vessel function and blood clotting abnormalities. Additionally, changes in skin texture and thickness can make the skin more susceptible to injury, leading to bruises.
Can medication affect bruising in diabetics?
Yes, certain medications like blood thinners, which are sometimes prescribed to diabetics, can increase the risk of bruising. These medications interfere with the body’s clotting process, making it easier to develop bruises from minor injuries.
What areas of the body are most prone to bruising in diabetics?
Diabetics often experience bruising on the shins, forearms, hands, and feet. These areas are more vulnerable to injury due to their frequent exposure to trauma and pressure.
People with diabetes should take extra precautions to protect these regions to reduce the likelihood of bruising.
Are there specific nutrients or supplements that can help prevent easy bruising in diabetes?
Consuming a diet rich in essential nutrients, especially vitamin C and vitamin K, can support overall skin health and minimize bruising. These vitamins play key roles in collagen production and blood clotting.
However, it’s essential to consult a healthcare provider before starting any supplements to ensure they are appropriate and safe for your specific condition.
When should diabetics be concerned about their bruising tendency?
Answer: Diabetics should be concerned if they notice frequent, severe, or unusual bruising not directly related to injuries or minor trauma. Such bruising may be a sign of underlying issues, and it’s important to consult a healthcare provider for an evaluation and guidance.
Conclusion
The propensity for diabetics to bruise easily is a lesser-known yet significant concern in the realm of diabetes-related complications.
Understanding the factors that contribute to this phenomenon is crucial for diabetic individuals and their healthcare providers.
While impaired blood vessel function, blood clotting abnormalities, skin changes, and other factors play a role, proper management of diabetes is key to reducing the risk of easy bruising.
This includes maintaining blood sugar levels within target ranges, staying hydrated, and protecting the skin from injury. Regular monitoring and early intervention for skin issues are also essential.
By addressing these factors and embracing a holistic approach to diabetes care, individuals with diabetes can minimize the impact of easy bruising on their quality of life and overall well-being.
Hi, I’m Mark Pattinson and I’m a freelance personal trainer. I’ve been working in the fitness industry for over 10 years especially since I work with diabetes patients and I love helping people achieve their fitness goals. I believe that everyone can benefit from a good workout, and I’ll do everything to make sure you get the most out of your training.